Comparing Medical Costs for Injured Workers Across 16 States
Cambridge, MA (PRWEB) October 16, 2014 -- The cost drivers of medical care in state workers’ compensation systems; the effects of legislative and regulatory changes on medical costs; and trends in payments, prices, and utilization of medical care for injured workers are examined in a new set of studies from the Workers Compensation Research Institute (WCRI).
The studies, CompScope™ Medical Benchmarks, 15th Edition, look at 16 different state workers’ compensation systems and provide a baseline of current medical costs and trends for policymakers and other stakeholders by documenting how medical payments per claim and their cost components compare over time with other states.
“The reports are indispensable for identifying where changes in treatment patterns may be occurring; where medical payments per claim or utilization may be atypical compared with other study states; or where, because of underutilization of medical services, there may be concerns about restrictions on access to care,” said Ramona Tanabe, WCRI's deputy director and counsel.
The studies cover the time period of 2007 to 2012, with claims' experience up through March 2013. The 16 states in the study—Arkansas, California, Florida, Illinois, Indiana, Iowa, Louisiana, Massachusetts, Michigan, Minnesota, New Jersey, North Carolina, Pennsylvania, Texas, Virginia, and Wisconsin—represent more than 60 percent of the nation’s workers’ compensation benefit payments. There are individual reports for all states except Arkansas and Iowa.
The following is a sample of the key findings found in the studies:
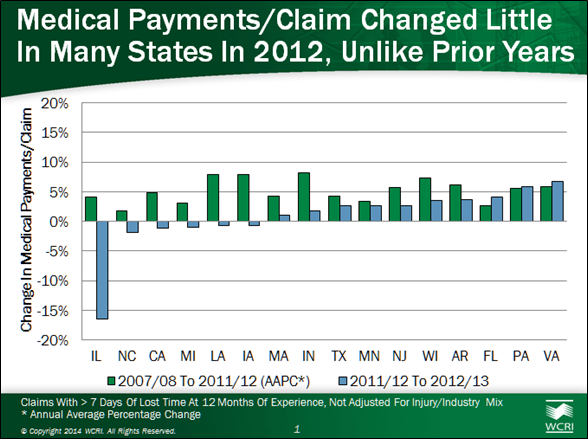
• Illinois: Medical payments per claim in Illinois fell 20 percent between 2010 and 2012, likely due to a reduction in the fee schedule rates.
• Texas: Overall medical costs per claim in Texas increased less than in many states from 2007 to 2012, reflecting 2005 reforms that took the state’s costs from the highest of the states that WCRI studied to one of the lowest.
• North Carolina: Hospital costs per claim in North Carolina remained higher than in most states, despite 2009 outpatient fee schedule changes that attempted to control those costs.
• Michigan: Medical costs per claim in Michigan grew more slowly than in the median of the 16 states WCRI studied. From 2007 to 2012, medical payments per claim grew 11.5 percent annually in Michigan, compared with 24.6 percent in the typical state.
The Cambridge-based WCRI is recognized as a leader in providing high-quality, objective information about public policy issues involving workers' compensation systems.
For more information about these studies, visit http://www.wcrinet.org/result/csmed15_all_result.html.
ABOUT WCRI:
The Workers Compensation Research Institute (WCRI) is an independent, not-for-profit research organization based in Cambridge, MA. Organized in late 1983, the Institute does not take positions on the issues it researches; rather, it provides information obtained through studies and data collection efforts which conform to recognized scientific methods. Objectivity is further ensured through rigorous, unbiased peer review procedures. WCRI's diverse membership includes employers; insurers; governmental entities; managed care companies; health care providers; insurance regulators; state labor organizations; and state administrative agencies in the U.S., Canada, Australia and New Zealand.
Andrew Kenneally, Workers Compensation Research Institute, +1 (617) 661-9274 Ext: 257, [email protected]
Share this article