Articles in the JACI Report Asthma Severity Phenotypes and Risk Factors in Inner-city Children
Milwaukee, WI (PRWEB) October 10, 2016 -- The Journal of Allergy and Clinical Immunology (JACI) has published three new articles about asthma severity in inner-city children. The reports work together to determine the risk factors that lead to asthma severity in the inner-city, distinguish what constitutes difficult-to-control asthma and categorize the severity “phenotypes” or types in the population.
“Pathways through which asthma risk factors contribute to asthma severity in inner-city children”:
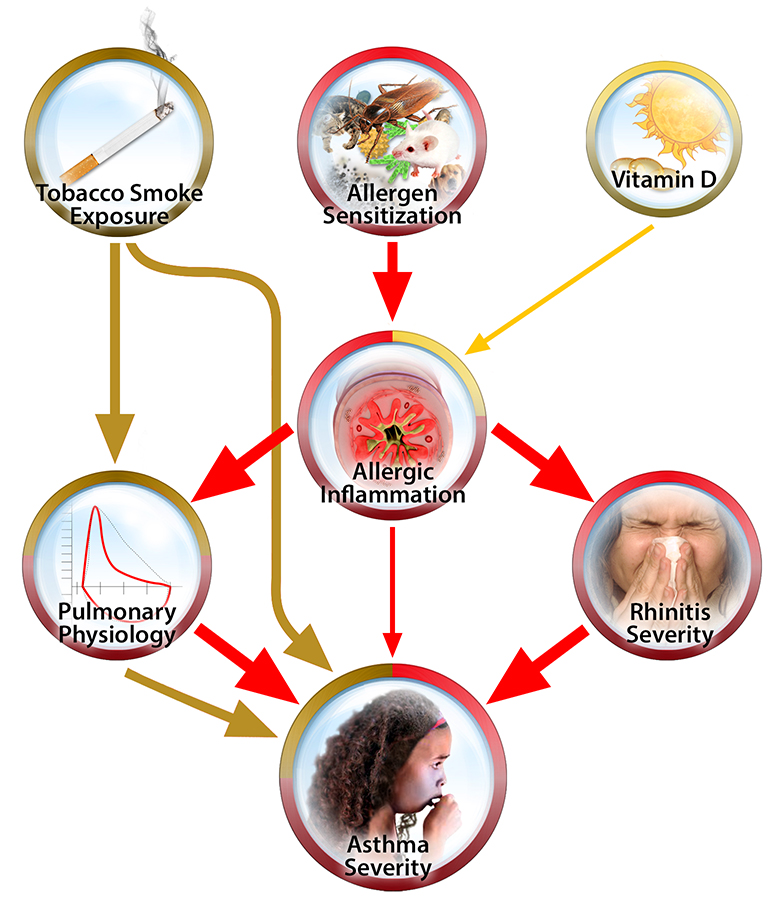
Children with asthma in inner-city areas have high burdens of symptoms and are more likely to die from the disease than children in other populations. The paper “Pathways through which asthma risk factors contribute to asthma severity in inner-city children” confirms asthma severity is caused by connected risk factors or “pathways.” The three most significant pathways identified are allergic sensitization, rhinitis and tobacco smoke exposure.
Allergic sensitization describes when someone becomes exposed and sensitized to the allergens in their environment. Common allergens in the inner-city environment include cockroaches, mice and mold. When a child is allergic to their environment, their lungs have more allergic inflammation and overall lung function and health decreases.
Rhinitis severity was also found to contribute to the severity of asthma. Rhinitis is a condition that causes inflammation in the nasal passages and a runny nose. Because children with severe rhinitis are unable to breathe through their nose, they breathe through their mouth. Since the air is not filtered as well as it would be through the nasal passages, lungs become more exposed to environmental triggers. Also, inflammation and congestion in the nose may cause coughing and directly irritate and affect the lungs.
Finally, tobacco smoke exposure puts children at risk. The smoke itself can be an irritant and it affects overall lung function and health, making asthma symptoms much more severe. The study measured children’s exposure to smoke by the number of adult smokers living in the home and the levels of cotinine, a byproduct of nicotine, in the children’s urine. Eighty percent of children in the study who did not have smoking adults in the home still tested positive for some smoke exposure.
Parental stress, obesity and vitamin D levels were also measured. While other research has found these to be factors relevant to asthma development and severity, they relatively small differentiators in this study.
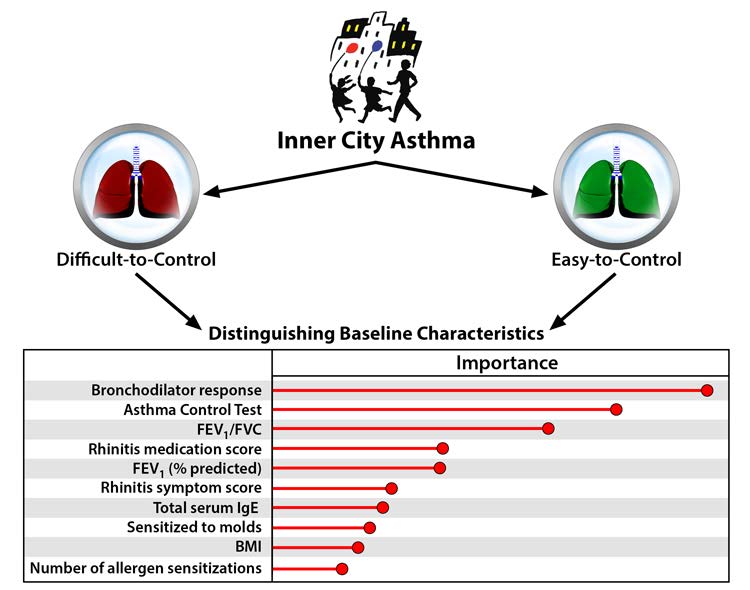
“Distinguishing characteristics of difficult-to-control asthma in inner-city children and adolescents”:
Researchers found the most significant markers of difficult-to-control asthma to be poor lung function, asthma control test scores and allergy. Despite good adherence to medication, difficult-to-control asthma had high exacerbation rates and showed little improvement in symptoms and lung function over the year the study took place, while easy-to-control asthma had the potential to improve.
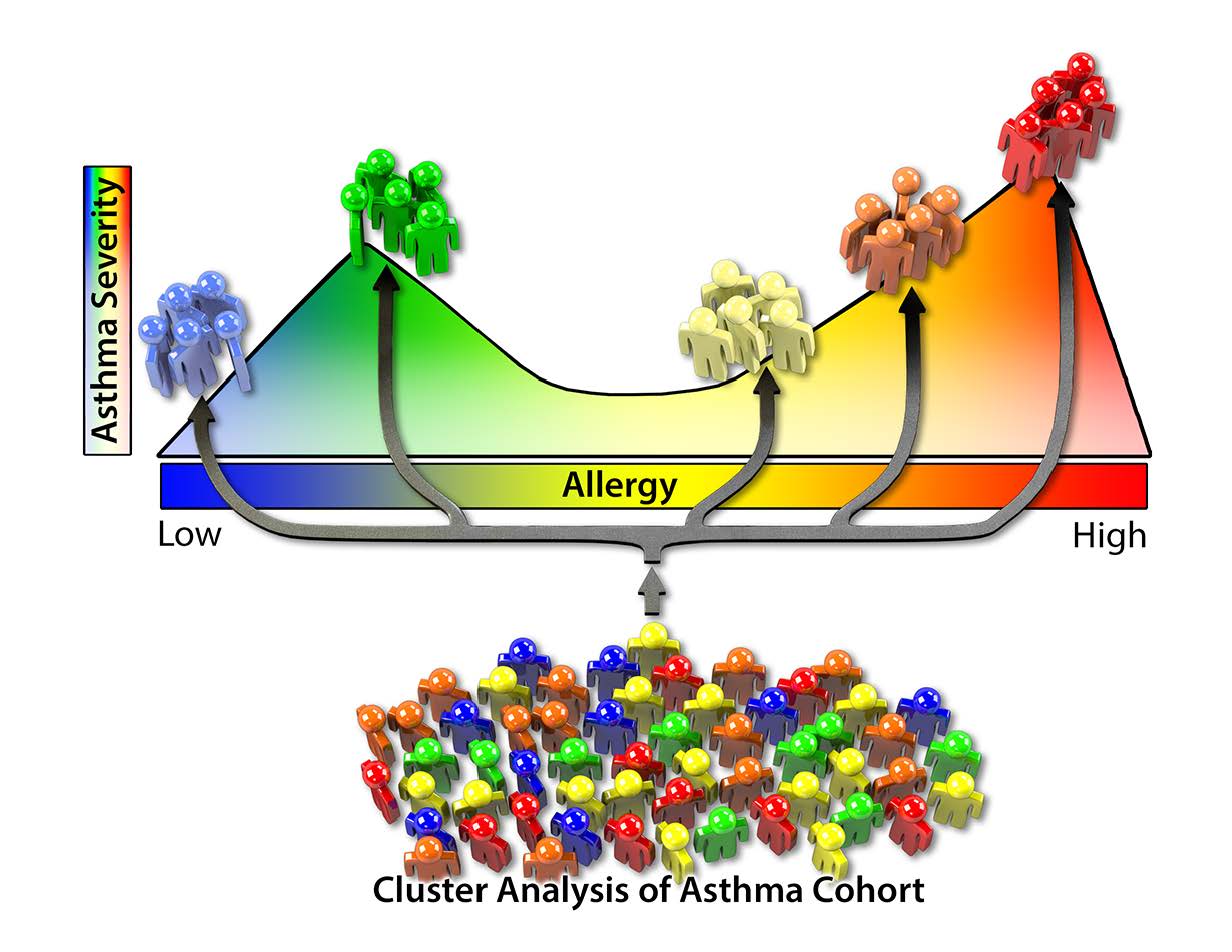
“Asthma phenotypes in inner-city children”:
Children were sorted into five different asthma phenotypes using a computer algorithm to determine how they “cluster.” Children who were in the two most severe groups made up 30.8% of the total sample group. Distinguishing asthma phenotypes could help doctors provide more personalized care.
“These three studies, taken together, can help clinicians and researchers identify and prioritize factors that influence asthma severity,” said Andrew H. Liu, MD, FAAAAI. “They can be used to form a roadmap for pathway-targeted intervention studies to improve future guidelines-directed care.”
The National Institute of Allergy and Infectious Diseases (NIAID) funded the work with additional support from the National Center for Advancing Translational Sciences, both parts of the National Institutes of Health (NIH). The Inner City Asthma Consortium, a nationwide clinical network supported by NIAID, conducted the research in nine U.S. cities.
The American Academy of Allergy, Asthma & Immunology (AAAAI) represents allergists, asthma specialists, clinical immunologists, allied health professionals and others with a special interest in the research and treatment of allergic and immunologic diseases. Established in 1943, the AAAAI has more than 6,900 members in the United States, Canada and 72 other countries. The AAAAI’s Find an Allergist/Immunologist service is a trusted resource to help you find a specialist close to home.
###
Rachel Maidl, The American Academy of Allergy, Asthma & Immunology, http://aaaai.org, +1 (414) 272-6071, [email protected]
Share this article