Study finds 30% Lower Cancer Risk with Vitamin D and Calcium
Encinitas, CA (PRWEB) April 17, 2017 -- In a study published March 28th in the Journal of the American Medical Association (JAMA),researchers at Creighton University found an inverse association between vitamin D serum levels and all non-skin cancer incidence. The analysis by vitamin D dosage showed a 30% reduction in the incidence of cancer (P=0.06). An analysis of the data by vitamin D serum level (vs dosage) showed that participants with vitamin D levels of 55 ng/ml vs those with 30 ng/ml were 35% less likely to get cancer (P=.03).
The serum level finding, however, was only reported in the supplemental material. The abstract and press release only reported the comparison by treatment group which found, “supplementation with vitamin D3 and calcium compared with placebo did not result in a significantly lower risk of all-type cancer.”
The key word in the finding by treatment group is “significantly.” No “significantly” lower risk does not mean that there was no compelling change, instead it has to do with statistics.
Significance in scientific research is a computation done during data analysis to evaluate the strength of the evidence. It is also called the P-value . In this paper it was reported in the abstract as, “A new diagnosis of cancer was confirmed in 109 participants, 45 (3.89%) in the vitamin D + calcium group and 64 (5.58%) in the placebo group (difference, 1.69% [95% CI, -0.06% to 3.46%]; P=.06)." This is a 30% reduction in cancer over 4 years, from day 0 to end, in the treatment group compared to the placebo group.
The P-value is a probability, it is a percentage. In this calculation the P-value was .06, which means that there is a 6% chance that the result (30% reduction in cancer in the vitamin D + calcium group) was due to chance - not the actual treatment. In a different wording, that means there is a 94% chance the reduction was due to vitamin D + calcium. The scientific community has agreed that P=.05 or less is the amount for study results to have "significance" and anything higher than P=0.05 is "not statistically significant." This arbitrary set point has no middle ground, it is black or white.
On page 7 of the paper, under 'Post Hoc Analyses,' when participants who withdrew from the study or developed cancer within the first 12 months were excluded from analysis, the study reported a 35% reduction in cancer risk in the vitamin D + calcium group compared to the placebo group with a P-value of 0.047. This was statistically significant.
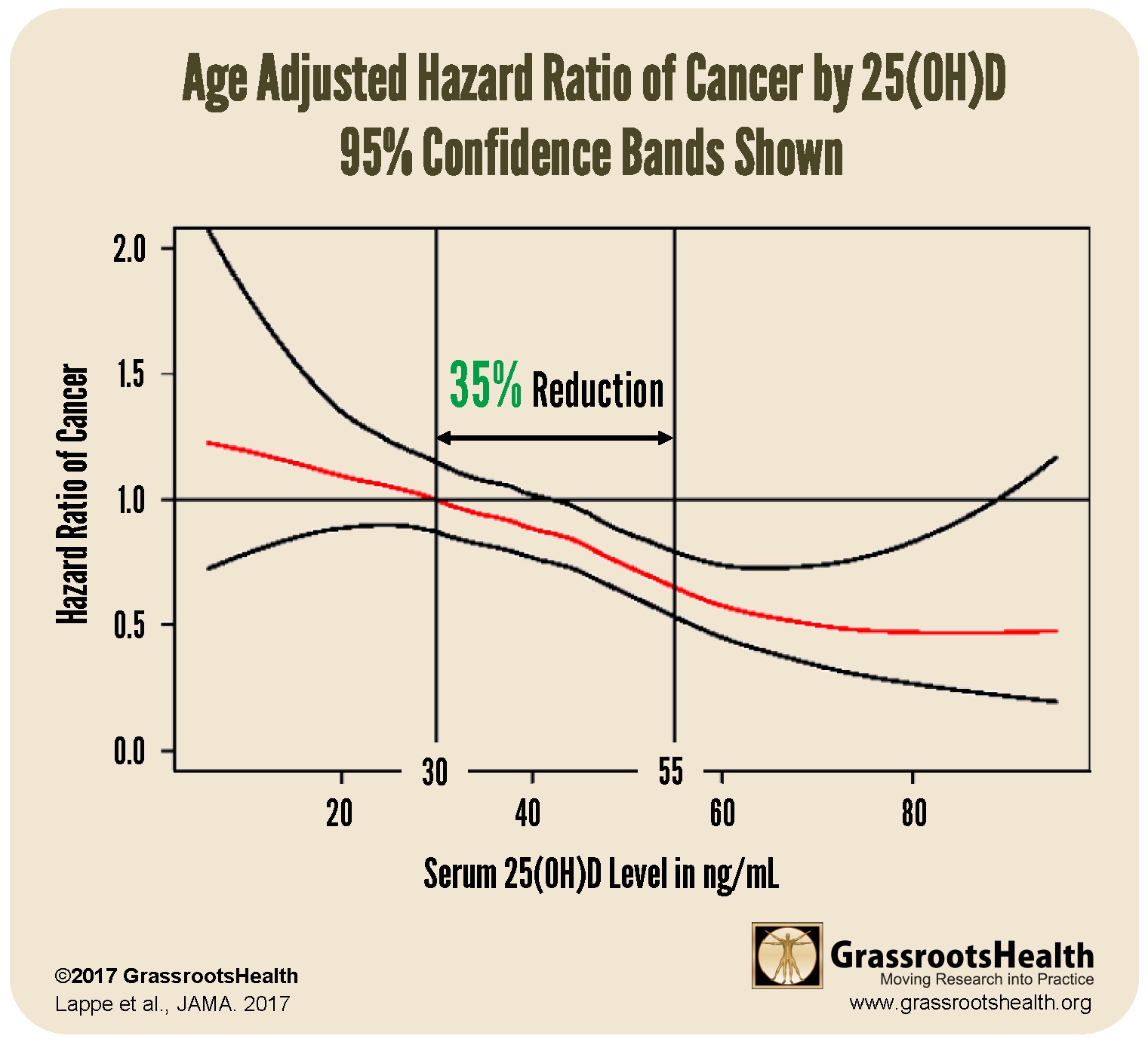
At GrassrootsHealth we recommend analyzing by serum level, the relevant biological marker for vitamin D. This analysis is also found in the section on Post Hoc Analyses, with the related chart in the supplementary online content of the JAMA article (most news outlets did not receive this chart). Analyzing by serum level showed that when compared with a vitamin D level of 30 ng/ml, participants with vitamin D levels of 55 ng/ml were 35% less likely to get cancer (P=0.03). This is statistically significant.
Analyzing by serum level also shows a trend that GrassrootsHealth is used to seeing - an inverse association between cancer incidence and vitamin D level, meaning that cancer incidence decreases as vitamin D levels increase.
“This 4-year randomized controlled trial replicated the outstanding randomized trial that investigators at Creighton University published in 2007. A total of 2303 participated in this study. It used a higher dose of vitamin D, 2000 IU/day vitamin D3, along with 1500 mg/day calcium,” said Cedric Garland, Dr PH FACE, Adjunct Professor at the UC San Diego School of Medicine, and co-investigator. ”Considering the average vitamin D level at entry to the study was 33 ng/ml, we are encouraged to see a 30-35% reduction in incidence of all invasive cancers combined. It is a compelling reduction in cancer incidence rates across all types of invasive cancer combined that cannot be achieved with anything else known to science but vitamin D."
“There has been a trend in the US to supplement with more vitamin D,” said Carole Baggerly, Director of GrassrootsHealth. “That is why it is critical to run a trial that not only tries to elicit a large change in serum 25(OH)D level in the treatment group, but to also analyze the results by its serum level. It was our own study of over 3,000 individuals that clearly demonstrated people metabolize vitamin D differently, so it is important to test levels and make conclusions on the level in the blood – not the amount ingested.”
About GrassrootsHealth
GrassrootsHealth is a non-profit public health research organization committed to moving vitamin D research into practice. Founded in 2007, when Director Carole Baggerly realized that vitamin D research existed that could possibly have prevented her breast cancer. GrassrootsHealth partners with 48 senior vitamin D researchers from around the world and spearheads methodologies for nutrient research like analyzing results by serum levels rather than oral intake of vitamin D. It disseminates vitamin D research findings to the public and public health officials.
Carole Baggerly, GrassrootsHealth, http://www.grassrootshealth.net, +1 (760) 579-8141, [email protected]

Share this article