Healthcare Companies Should Expect Increased Fraud Enforcement in 2021
Bass, Berry & Sims' Healthcare Fraud & Abuse Review 2020: Scrutiny of receipt of COVID-19 relief funds likely to lead the way amid increased enforcement focus across all healthcare sectors.
NASHVILLE, Tenn., Feb. 5, 2021 /PRNewswire-PRWeb/ -- Examining issues surrounding the receipt of COVID-19 relief funds will be a significant area of focus for the government as it ratchets up scrutiny of healthcare companies in 2021, according to Bass, Berry & Sims' ninth annual Healthcare Fraud & Abuse Review 2020.
The federal government's financial response to the pandemic through the CARES Act and other COVID-19 relief programs has allocated billions of dollars to the healthcare industry. The Review details how such a scenario presents an enforcement perfect storm for the healthcare industry as a result of the distribution of large amounts of fast cash within a highly regulated industry, along with poor and evolving government guidance, and assured retrospective scrutiny by the regulators.
Download the Healthcare Fraud & Abuse Review 2020.
"The federal government has already moved to shut down blatantly fraudulent schemes related to the CARES Act and COVID-19 relief. We expect the government to shift its attention to the billions of dollars earmarked for hospitals and other healthcare providers, scrutinizing eligibility, use and documented support for COVID-19 funds," said Brian D. Roark, head of the Bass, Berry & Sims Healthcare Fraud Task Force. "We expect these investigations will be much more wide-ranging than more typical fraud investigations in healthcare. Regulators examining the need and use of COVID-19 relief funding are likely to scrutinize the whole enterprise."
Recoveries down, new cases up
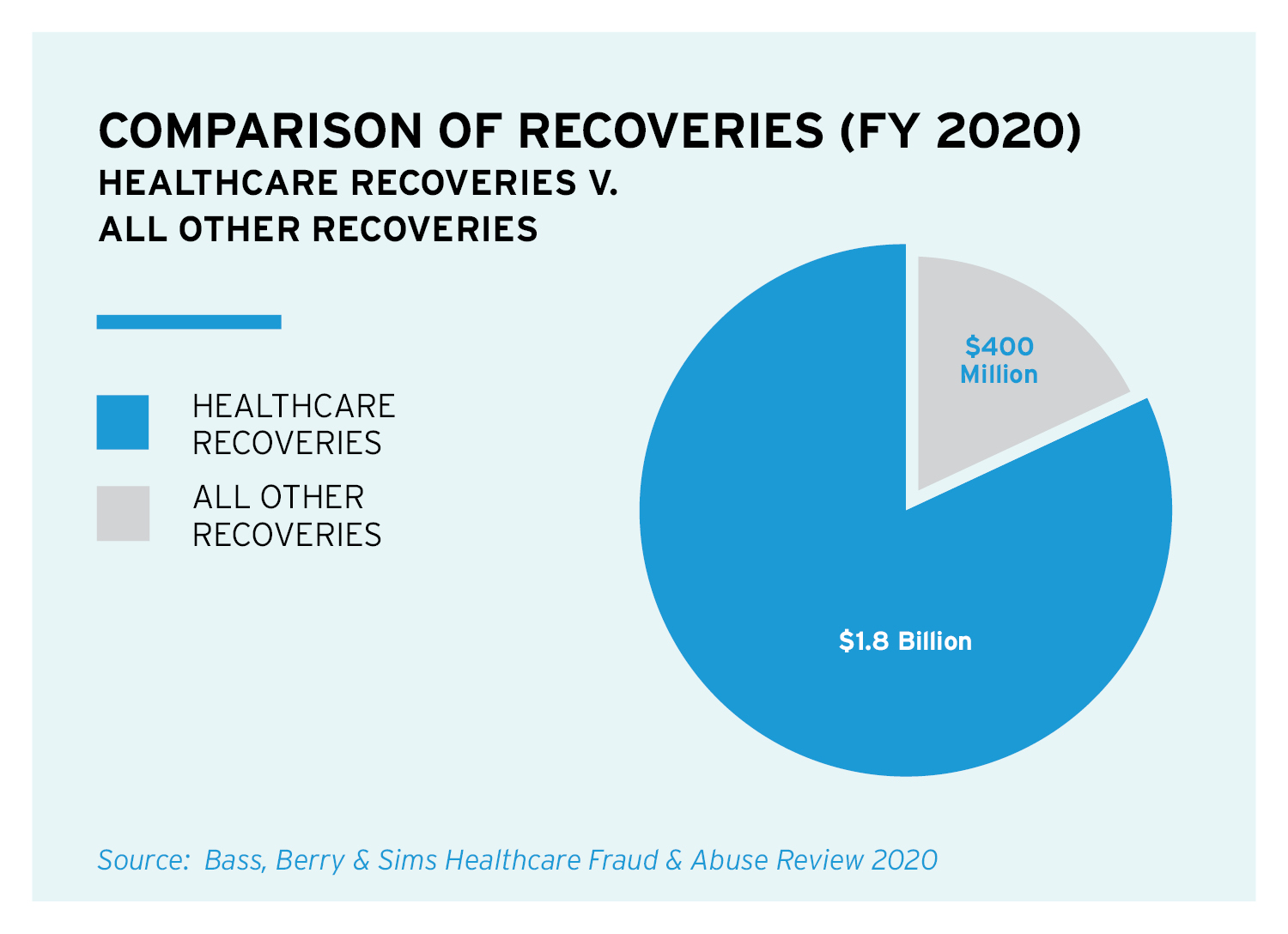
The raw numbers suggest that the pandemic impacted investigations, litigation and civil fraud recoveries during federal fiscal year 2020, which ended Sept. 30, 2020. Recoveries by the U.S. Department of Justice (DOJ) in FY20 declined nearly 30 percent compared with the prior fiscal year, dropping to $2.2 billion from the $3.1 billion collected in FY19. Notably, the $2.2 billion in civil fraud recoveries is the lowest amount recovered in more than 10 years. One thing that has not changed, however, is the fact that recoveries from healthcare-related cases continued to comprise the overwhelming percentage of total recoveries, amounting to more than $1.8 billion of the total.
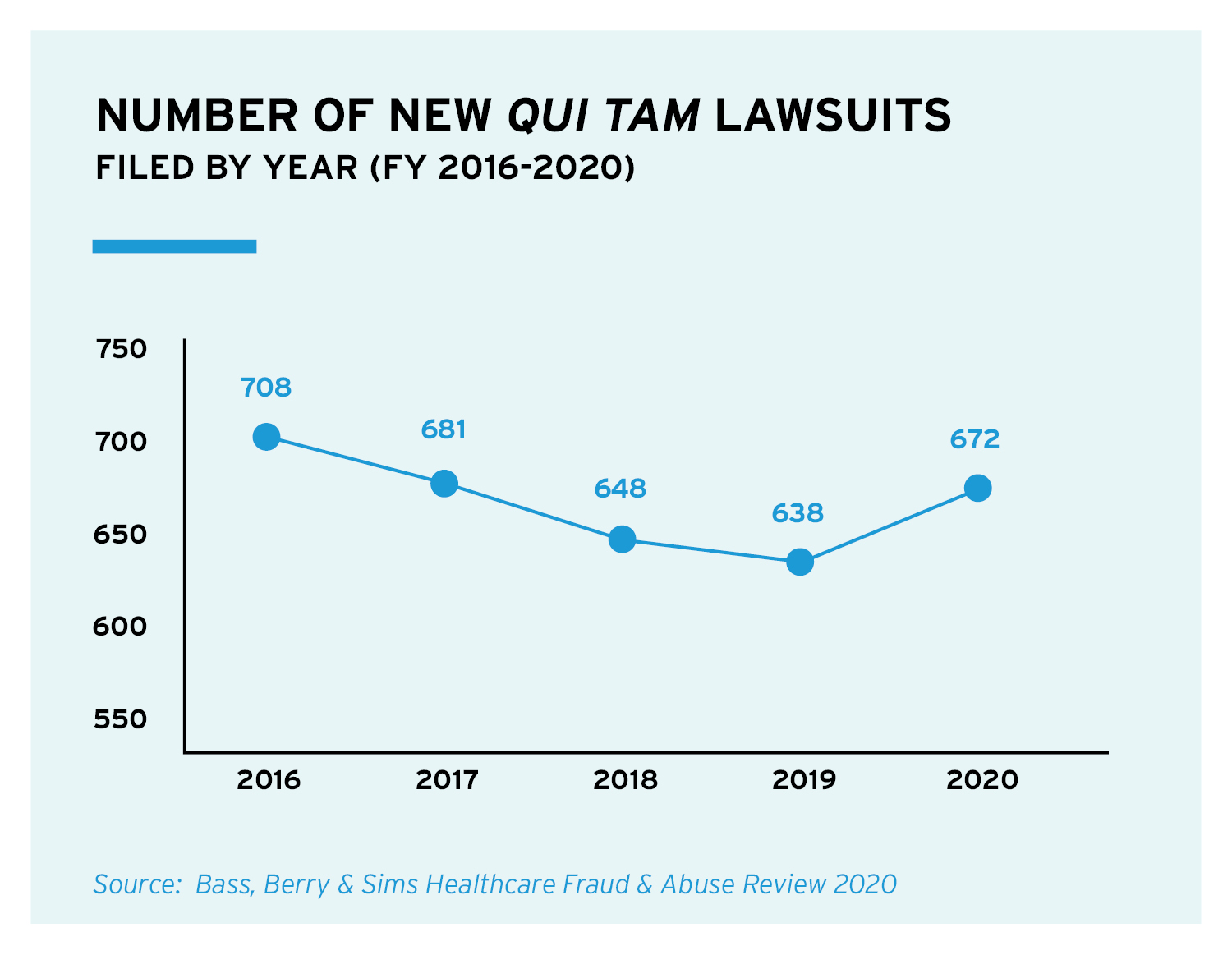
Announced recoveries in FY21 already have eclipsed the 2020 total and are nearing $4 billion, fueled by a number of high-profile opioid-related settlements. New qui tam lawsuits filed under the False Claims Act in FY20 increased to 672 new cases and another 250 non-qui tam civil fraud suits were filed, representing an increase of more than 100 compared with FY19, according to DOJ figures. The significant number of new cases will continue to fuel enforcement efforts for years to come.
"The early days of the pandemic may have delayed enforcement efforts somewhat, but the activity toward the end of last year and so far this year suggests the lull is over," said Matthew M. Curley, a member of the firm's Healthcare Fraud Task Force and lead editor of the Healthcare Fraud & Abuse Review. "Since 2010, more than 7,000 whistleblower cases have been filed under the False Claims Act, and whistleblowers have collected nearly $4.2 billion for their efforts during those years. There can be no question that the financial incentives to file qui tam whistleblower lawsuits remain compelling."
Sectors and issues to watch
For hospitals and health systems, regulators and whistleblowers continued their focus on issues arising under the Anti-Kickback Statute and the Stark Law. Scrutiny of financial arrangements between hospitals and physician referral sources resulted in a number of high-profile False Claims Act settlements last year. "Management services agreements and alleged physician inducements continue to receive significant scrutiny from regulators and whistleblowers," said Anna M. Grizzle, a member of the firm's Healthcare Fraud Task Force who advises clients in connection with enforcement and compliance-related issues. "These settlements are a reminder that even during an unprecedented pandemic, healthcare providers cannot afford to lose focus on the importance of ensuring their relationships with referral sources are compliant with the applicable regulations."
The pharmaceutical and medical device industries continued to account for the largest recoveries within the healthcare industry last year. Many of the headliner settlements related to the opioid crisis and many involved allegations of Anti-Kickback Statute violations. The government also stepped up its scrutiny of payments to physicians for speaking engagements where payments were intended to induce prescriptions. In what is surely a sign of things to come, HHS-OIG issued a Special Fraud Alert on speaker programs, highlighting the risks such programs pose.
"Enforcement actions involving speaker programs reflect a growing focus by regulators on the relationship between pharmaceutical and medical device manufacturers and providers," said John E. Kelly, managing partner of Bass, Berry & Sims' Washington, D.C., office and former Assistant Chief for Healthcare Fraud at the DOJ. "HHS-OIG and the DOJ are routinely looking closely at both sides of these relationships—in this case, manufacturer and provider—and this is a clear reminder to the industry that the Anti-Kickback Statute is a two-way street. For providers, the old adage rings true: If an offer sounds too good to be true, it probably is."
Last year also saw continued efforts to pursue civil and criminal enforcement against individuals in fraud cases. Physicians and healthcare executives settled civil and criminal allegations related to medical necessity, services not provided, inflated bills, kickbacks and other allegedly fraudulent activity. Two executives were part of a $41 million settlement resolving allegations of submitting false claims for presumptive and definitive urine drug testing that was not medically reasonable or necessary.
"Holding individuals accountable in healthcare fraud cases is now a well-established fraud enforcement priority," said Lisa S. Rivera, a Healthcare Fraud Task Force member and former federal prosecutor. "The increased liability of executives for corporate actions makes the need to lead on compliance all the more personal. Making this a top leadership priority within an organization is a critical element of building and maintaining a culture of compliance."
For long-term-care facilities, the focus of regulators and whistleblowers likely will turn to fraud theories related to quality of care. For its part, DOJ announced its National Nursing Home Initiative in furtherance of its previously announced Elder Justice Initiative and has forecast increased civil and criminal enforcement efforts focused on nursing homes where grossly substandard care to residents has been provided.
"The current COVID-19 crisis will accelerate regulators' focus on quality-of-care issues," said Jeff H. Gibson, a member of the Healthcare Fraud Task Force. "Whistleblowers recognize this reality and likely will be pursuing cases based on inadequate care. Skilled-nursing providers must closely monitor quality metrics and complaints regarding quality and work to address identified shortcomings proactively."
Comprehensive review of settlements
Bass, Berry & Sims' Healthcare Fraud & Abuse Review 2020 will assist healthcare companies in developing a greater understanding of the civil and criminal enforcement risks they face during a time of great uncertainty for the healthcare industry. The Review offers analysis of major trends in False Claims Act case law, issues to watch as 2021 unfolds, and a comprehensive review of settlements in the following categories:
- Hospitals and Health Systems
- Hospice and Home Health
- Skilled Nursing Facilities and Nursing Homes
- Pharmaceutical and Device
- Laboratory, Pathology, Radiology and Diagnostics
- Behavioral Health and Substance Abuse Treatment
- Specialty Care and Other Provider Entities
- Individual Providers
- Other
Download the Review here and visit Bass, Berry & Sims' Inside the FCA blog to stay up-to-date on FCA matters.
About Bass, Berry & Sims PLC
With nearly 300 attorneys representing numerous publicly traded companies and Fortune 500 businesses, Bass, Berry & Sims has been involved in some of the largest and most significant litigation matters, investigations and business transactions in the country. For more information, visit http://www.bassberry.com.
Media Contact
Tracy Roberts, Marketing & Communications Director, Bass, Berry & Sims PLC, +1 (615) 259-6330, [email protected]
SOURCE Bass, Berry & Sims PLC

Share this article